When BarkingDogShoes.com founder Kirsten Borrink talks about finding the right shoes for women with rheumatoid arthritis (RA) the answers are personal. Borrink herself faced sudden-onset RA at the age of 27. The condition left her almost unable to work in the teaching career she loved. Blogging about the experience she writes: “Rheumatoid Arthritis has caused more structural changes in my feet than anywhere else…I don’t particularly like talking about bunions, hammertoes, fallen arches and such, but it’s what I live with and what motivates me to continue to search out the best in comfort footwear.”
Her struggle to find shoes that fit and eased her pain led her to launch a shoe blog profiling comfortable stylish shoes for women with problem feet. Borrink has shared her story and shoe advice in publications like Arthritis Today Magazine, and Today.com. Whether you’ll new to RA or looking for shoes to help your long-aching feet, here is some info on the causes and symptoms of RA and some comfortable, stylish shoes that may help keep you moving.

Kirsten, founder of BarkingDogShoes.com, wears Fitflop sneakers—
a great choice for aching feet due to RA, bunions, metatarsalgia.
What is Rheumatoid Arthritis
Contrary to popular belief rheumatoid arthritis is not a disease that only older people get. Borrink remembers the isolation she felt after her RA diagnosis when people said she was too young to have RA. “One of the most frustrating aspects of the disease, right up there with fatigue and pain, was loneliness. Comments from well-meaning co-workers like, “Oh, you’re too YOUNG for arthritis,” or “My grandma has that,” only served to further those well-remembered feelings of isolation.”
Rheumatology.org (a website for those docs who are experts in diseases such as arthritis) says RA “affects more than 1.3 million Americans. About 75% of RA patients are women.” And they say the disease most often occurs between the ages 30-50, hardly a disease of grandparents.
So what is rheumatoid arthritis? According the American Academy of Orthopaedic Surgeons, “Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often starts in the small joints of the hands and feet, and usually affects the same joints on both sides of the body.” Experts say early on it may not affect joints on both sides of the body but will if someone’s had it for awhile.

The actual suede Hush Puppies shoes Kirsten was wearing the day her RA pain started.
She’s kept them as reminder of the day her health changed drastically.
Causes of Rheumatoid Arthritis
RA is known as an autoimmune disease. That means for some reason the body’s immune system starts viewing healthy tissue or joints as ‘the enemy’ and the body literally attacks itself. According to AAOS, “In RA, the defenses that protect the body from infection instead damage normal tissue (such as cartilage and ligaments) and soften bone.”
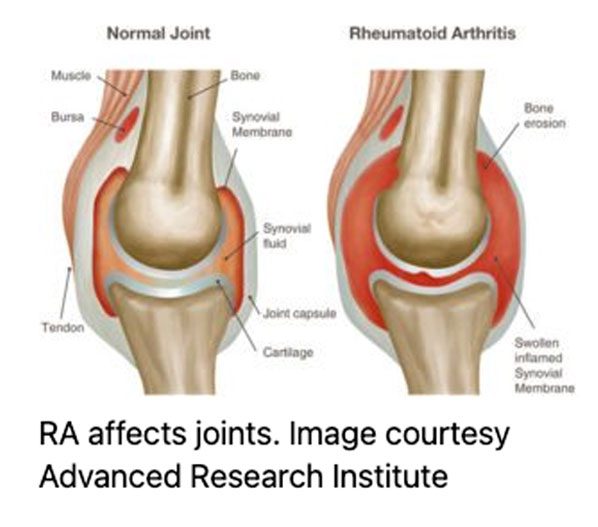
The experts at the Johns Hopkins Arthritis Center say there’s a lining that covers your joints called the synovium which gives nutrients to your cartilage and helps maintain synovial fluid. This nasty arthritis makes that cover swell up which can destroy the surrounding joint by invading nearby cartilage and bone areas. It actually activates the tiny cells that destroy bone tissue during normal healing.
The exact cause of RA is still unclear. Its thought to be a combination of your genes, environmental factors (possibly smoking and maybe even the bacteria that cause gum disease) but also some sort of trigger that sets off RA. Per AAOS, “There is usually a ‘trigger’ which activates the genes. When the body is exposed to this trigger, the immune system responds inappropriately. Instead of protecting the joint, the immune system begins to produce substances that attack the joint.”
Symptoms of Rheumatoid Arthritis
Symptoms of RA can be similar to other autoimmune diseases or other types of arthritis. They may include:
- Swelling joints in fingers and feet
- Pain and tenderness
- Stiffness in the morning for 30 minutes to an hour. Rheumatology.org says this morning soreness can help doctors figure out if it is RA versus other types of arthritis. “The joint stiffness in active RA is often the worst in the morning. It may last one to two hours (or even the whole day). It generally improves with movement of the joints. Stiffness for a long time in the morning is a clue that you may have RA, as this is not common in other conditions.”
- Joints may feel warm to the touch
- Moving your joints may hurt
- Lumps (even bony growth) under the skin
- Fatigue
- Lack of appetite
- Eye swelling
- Low grade fever (99-100 degrees)
- Same joints on both sides of the body are affected
Test and Treatment for RA
Unfortunately there is no cure. It is important to get tested and treated for RA. For example, the Johns Hopkins Arthritis Center writes “RA causes joint damage in 80% to 85% of patients, with the brunt of the damage occurring during the first 2 years of the disease.” Experts say it can also shorten the life of patients if left untreated due to the possibility of cardiac complications.
Experts say treatment can stop pain and swelling and prevent joint damage. If you suspect you have RA you should consult a rheumatologist or orthopaedic surgeon (sometimes the first stop before a rheumatologist is involved). Your doctor may perform a careful examination of your joint and conduct tests to help diagnose RA. Doctors may take x-rays, or even use ultrasounds or MRI testing to look for joint damage. In addition, blood tests may look for Rheumatoid factor (RF) or also an anti CCP test. Experts say up to 80% of RA patients may test positive for RF.
Treatments for your RA may include medications, reducing stress on your joints with things like ice, non steroidal anti-inflammatories, braces and even custom orthotics. A treatment course may also involve physical and occupational therapy, and sometimes surgery. For instance, Borrink eventually elected to have surgery to fuse the bones in her forefoot after RA damaged the area. Not great to have surgery but it removed her need to wear custom orthotics at the time.
Rheumatoid arthritis in feet
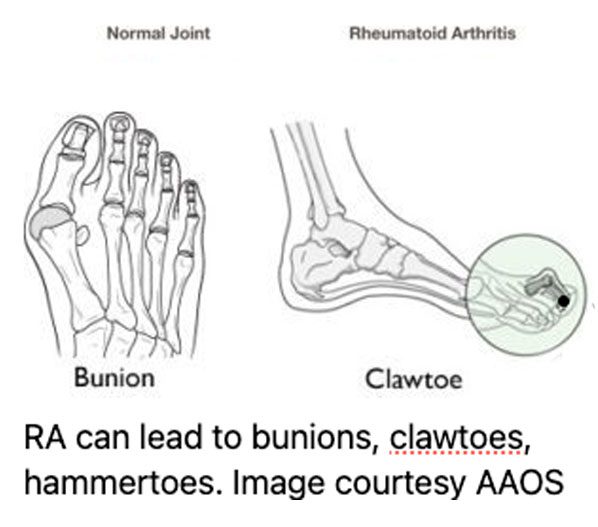
If you have RA your feet and ankles may be one of the first to let you know. In about 20% of patients foot and ankle symptoms are the first sign of RA according to AAOS. And almost all people with RA will develop symptoms in their foot or ankle over time. Borrink said her RA affected her feet the most and led to a number of problems including affecting her ability to buy typical shoes. She contributed to an article about shoes and RA for Arthritis Today Magazine: “But if you do have arthritis today like I do, I’m guessing you’ve suffered some structural changes to the forefoot causing myriad problems such as hammertoes, neuroma, metatarsalgia, and those straight-from-the-pit-of-hell bunions.” So yes, in addition to achy feet, people who have RA may experience other foot problems such as:
- hallux rigidus. Does it surprise you to learn the base of your big toe is actually the most common site of arthritis in your feet? The joint has to bend every time you step. Learn more in our Comprehensive guide to hallux limitus/rigidus.
- Morton’s Neuroma – This can flare when arthritis swollen joints are kept in shoes that are now too tight in the forefoot. Changing footwear can help.
- Did you know RA can mimic plantar fasciitis? According to podiatrynetwork.com “Rheumatoid arthritis can be a source of pain on the bottom of the heel. This can mimic the classical heel pain caused by plantar fasciitis. It is important for the treating doctor to consider Rheumatoid arthritis as a cause of heel pain.” We’ve got plenty of shoes and sandals to help with the ouch of plantar fasciitis as well.
- fallen arches (osteopenia)
- hammertoes and bunions
When you have RA your footwear choices can make a big difference. That same Arthritis Today article quotes a Harvard expert who says “Making healthy choices for your feet, much like eating a nutritious diet or getting regular exercise, can add up to big improvements in quality of life… People should start thinking of their shoes as a factor they can modify to help minimize pain and maximize their ability to get out and do things.”
The wrong shoes are not only uncomfortable but they may aggravate joint problems, bunions, hammertoes, neuromas, even further. So what should you look for in shoes if you have rheumatoid arthritis? Borrink always recommends a lower heel, no more than 1 – 1.5 inches. Keep in mind some supportive platform shoes may allow you to wear a higher ‘heel’ while keeping your foot supported.
Webmd.com also recommends shoes with a wide toe box. Note: You may need a larger size than before you developed arthritis. In addition to swollen joints, some people with RA develop nodules on the sides of their foot or toes. Also, consider avoiding shoes with laces. RA flare ups may leave hands swollen making it difficult to tie shoes.
So where to start when looking for shoes? A good place might be our blog post on The Best Shoe Styles from 5 Comfort Brands. This post can introduce you to some of the best-known comfort shoe makers such as Dansko and point you to a few styles that might be a good starting point in your journey to find shoes that make daily life a little more bearable. In addition, barkingdogshoes.com has the option to search by foot condition types so you can find shoes for bunions, hallux rigidus, Morton’s Neuroma and other conditions that may impact your feet if you have RA.
You might also enjoy an on-the-go oxford from Arcopedico with a knit upper that works for bunions and hammertoes.
Finally, take a look at a few of the shoes we love that have also earned the APMA seal.
Walking shoes for RA
One of the things that sounds awful to some in the throngs of an arthritis flair, walking, may actually be helpful. “Regular low-impact exercises, such as walking, and exercises can increase muscle strength. This will improve your overall health and lower pressure on your joints,” according to rhuematology.org. Over the years Kirsten tried to move beyond walking but her RA has brought her back to this dependable exercise. “I’ve tried jogging and love the cardiovascular workout and endorphin rush, but my knees nixed that crazy endeavor, as did my rheumatologist. So I returned to what I do best: I walk. While my friends do crossfit, hot yoga, early spin classes and kick-boxing, I walk. I really do wish I could participate in those activities to challenge myself, but I know my limits. So I walk. It’s something I can do with relatively little pain, hopefully for a long while.”
As a result, we’ve devoted many posts to the best supportive comfortable walking shoes. Such as this one on the best walking shoes for women. Whether you need help with shoes for a hammertoe, plantar fasciitis or even walking shoes that don’t look like walking shoes, you’ll find choices on our blog.
We want to hear from you
We hope you’ve learned more about rheumatoid arthritis. If you have shoes or boots that you’ve found help with your RA-related foot problems, please share! We also have an active community of readers and tips on our Facebook page.
Related Resources
Arthritis Foundation Arthritis.org – rheumatoid arthritis information page
Arthritis Today Magazine article – includes tips from Kirsten Borrink
everydayhealth.com Best shoes for rheumatoid arthritis. also includes tips from Kirsten Borrink
Johns Hopkins Arthritis Center – rheumatoid arthritis information for patients and clinicians
OrthoInfo rheumatoid arthritis page – American Academy of Orthopaedic Surgeons (AAOS) patient information
OrthoInfo rheumatoid arthritis of the foot and ankle – AAOS patient information page specifically addressing RA in the foot and ankle
Rheumatology.org – American College of Rheumatology patient information pages
Webmd.com – Arthritis footcare and shoe informaNote: the above content is not intended to be medical advice or substitute for seeking the advice of a qualified medical professional. We’re talking shoes here.







Leave a Reply